The Link Between Gum Disease and Diabetes
Why healthy gums matter when you’re managing blood sugar—and how dental care can support your overall health

Most people think of diabetes as a condition that affects blood sugar, energy, and overall health. What many patients do not realize is that diabetes can also have a major impact on the gums. In fact, the relationship goes both ways: diabetes can increase the risk of gum disease, and gum disease can make diabetes harder to manage.
That connection is one reason why gum health should be part of every diabetes care plan. If you have diabetes—or you have been told you are at risk—it is important to understand how your oral health fits into the bigger picture.
What Is Gum Disease?
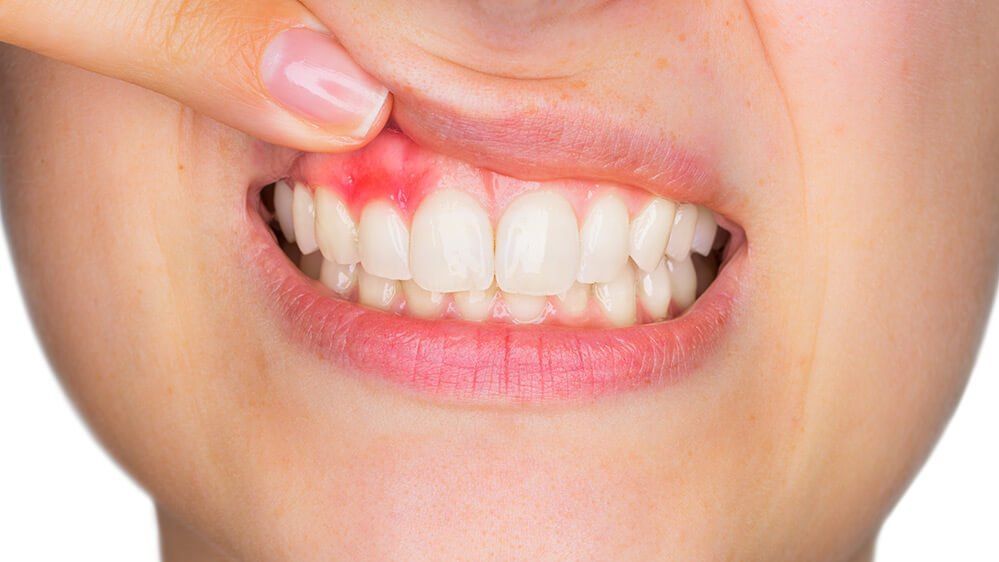
Gum disease, also called periodontal disease, is an infection and inflammatory condition that affects the gums and the tissues that support the teeth. It often begins as gingivitis, which can cause redness, swelling, and bleeding. If it is not treated, it can progress into periodontitis, where the infection and inflammation can damage the bone and tissues that hold teeth in place. In more advanced cases, gum disease can lead to loose teeth, discomfort, chewing problems, and tooth loss.
One of the challenges with gum disease is that it may not feel severe in the beginning. Many people ignore occasional bleeding when brushing or flossing, but that is often an early warning sign that something is wrong.
How Diabetes Affects Gum Health
Diabetes can make it easier for gum disease to develop and harder for the body to fight it off. When blood sugar levels stay elevated, the body may be more vulnerable to infection, inflammation can become more severe, and healing may take longer. People with diabetes may also experience dry mouth, which can contribute to bacterial buildup and other oral health problems.
This means patients with diabetes are not just slightly more likely to have gum problems—they may also experience more severe periodontal issues if those problems are left untreated. The American Academy of Periodontology notes that people with diabetes are more likely to develop periodontal disease than those without diabetes.
How Gum Disease Can Affect Diabetes
The connection is not one-sided. Gum disease may also make diabetes more difficult to control. Periodontal disease is an inflammatory condition, and ongoing inflammation in the body can work against blood sugar management. That is why researchers and major health organizations describe the relationship between diabetes and gum disease as a two-way one.
In practical terms, that means untreated gum disease may add another obstacle for patients who are already trying to keep their glucose levels in a healthy range. Treating gum inflammation and infection may help support better diabetes management as part of a broader care plan that also includes medical care, diet, and healthy habits.
Signs to Watch For
If you have diabetes, it is especially important to pay attention to symptoms that could point to gum disease.
These may include:
- Red, swollen, or tender gums
- Bleeding when brushing or flossing
- Persistent bad breath
- Gum recession or teeth that look longer
- Loose teeth
- Pain when chewing
- Changes in the way your teeth fit together
You may also notice dry mouth or slower healing after irritation in the mouth, which can be more common in people with diabetes.
Why Early Treatment Matters
Catching gum disease early gives patients the best chance of controlling it before it causes deeper damage. Gingivitis, the earliest stage of gum disease, is generally treatable and reversible with professional care and good home hygiene. Once gum disease advances and begins affecting the supporting bone and deeper tissues, treatment becomes more involved.
For patients with diabetes, early treatment matters even more because healing may be slower and infection can have a greater impact on the body. Addressing gum problems early can help protect your smile and reduce one more source of chronic inflammation.
How to Protect Your Gums if You Have Diabetes
The good news is that there are clear steps you can take to lower your risk and protect your oral health.
Keep blood sugar as well controlled as possible
Good diabetes management supports your entire body, including your gums. When blood sugar is better controlled, the body is generally in a better position to fight infection and heal properly.
Brush and clean between your teeth every day
Daily plaque removal is essential. Brushing thoroughly and cleaning between teeth with floss or another recommended tool helps reduce the bacteria that contribute to gum disease.
Stay consistent with dental visits
Regular cleanings and gum evaluations are especially important for patients with diabetes. Professional care can catch early signs of inflammation before they become more serious. The NIH and ADA both emphasize regular dental care for people with diabetes.
Do not ignore bleeding gums
Many patients assume bleeding is normal if they brush hard, but healthy gums should not bleed regularly. Bleeding can be an early sign of gingivitis or periodontal disease.
Share your medical history with your dental team
Your dentist should know if you have diabetes, if your blood sugar has been difficult to manage, or if you are taking medications that may affect your mouth. That information helps guide the right preventive and treatment approach.
When to Schedule a Periodontal Evaluation
If you have diabetes and you are noticing bleeding gums, bad breath, gum tenderness, recession, or loose teeth, it is a good idea to schedule an evaluation sooner rather than later. Even mild symptoms can point to the beginning of gum disease.
At Aurora Dental Care, we help Seattle patients identify gum problems early and recommend treatment based on the severity of the condition. Whether the issue is mild gingivitis or more advanced periodontal disease, timely care can make a meaningful difference for your oral health and your overall wellness.
Final Thoughts
The link between gum disease and diabetes is too important to ignore. Diabetes can raise the risk of periodontal problems, and periodontal disease can make blood sugar management more challenging. Taking care of your gums is not just about protecting your smile—it is part of taking care of your whole body.
If you have diabetes and have noticed changes in your gums, scheduling a dental evaluation is a smart next step. Early care, consistent hygiene, and ongoing monitoring can go a long way toward keeping both your mouth and your health on track.